CCBHC Adoption
Washington is facing a community behavioral health care crisis. Funding that requires annual stopgap rate increases and still doesn’t compensate for many essential services, compounded by 30-40% increases in service requests and continually escalating operational costs have put unsustainable pressures on what should be a thriving system.
We need a sustainable, long-term solution.
Introducing Certified Community Behavioral Health Clinics or CCBHCs:
What are Certified Community Behavioral Health Clinics?
CCBHCs encompass several important elements that make it more effective and sustainable than our current system:
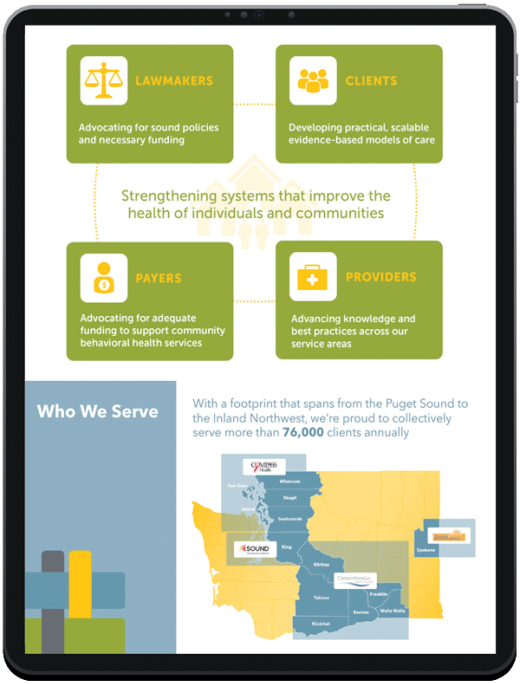
- Holistic clinical model – CCBHCs integrate mental and physical health services to promote whole-person care by delivering comprehensive behavioral health services and substance use treatment and prioritizing care coordination to connect clients to physical health care services, as well.
- Sustainable payment structure – The distinctive funding model under which CCBHCs operate enables providers to forecast community needs and secure adequate funding for all services provided, including preventive and engagement services that providers are currently delivering for free because there’s no billing code for them.
- Robust quality-of-care reporting – CCBHCs establish a pipeline of data reporting that supports population-wide visibility into trends and interventions to support more informed decision-making at a large scale.
CCBHCs provide a central access point for mental health care, substance use treatment and screenings on the social determinants of care. They mirror Federally Qualified Health Centers (FQHCs), which for decades have successfully delivered medical care to low-income community members who qualify for Medicaid benefits.
By creating parity between our behavioral health and medical system, the CCBHC model helps to ensure everyone in our communities with access to the care they need, regardless of their ability to pay or the severity of their diagnosis.
Why are CCBHCs the solution for Washington state?
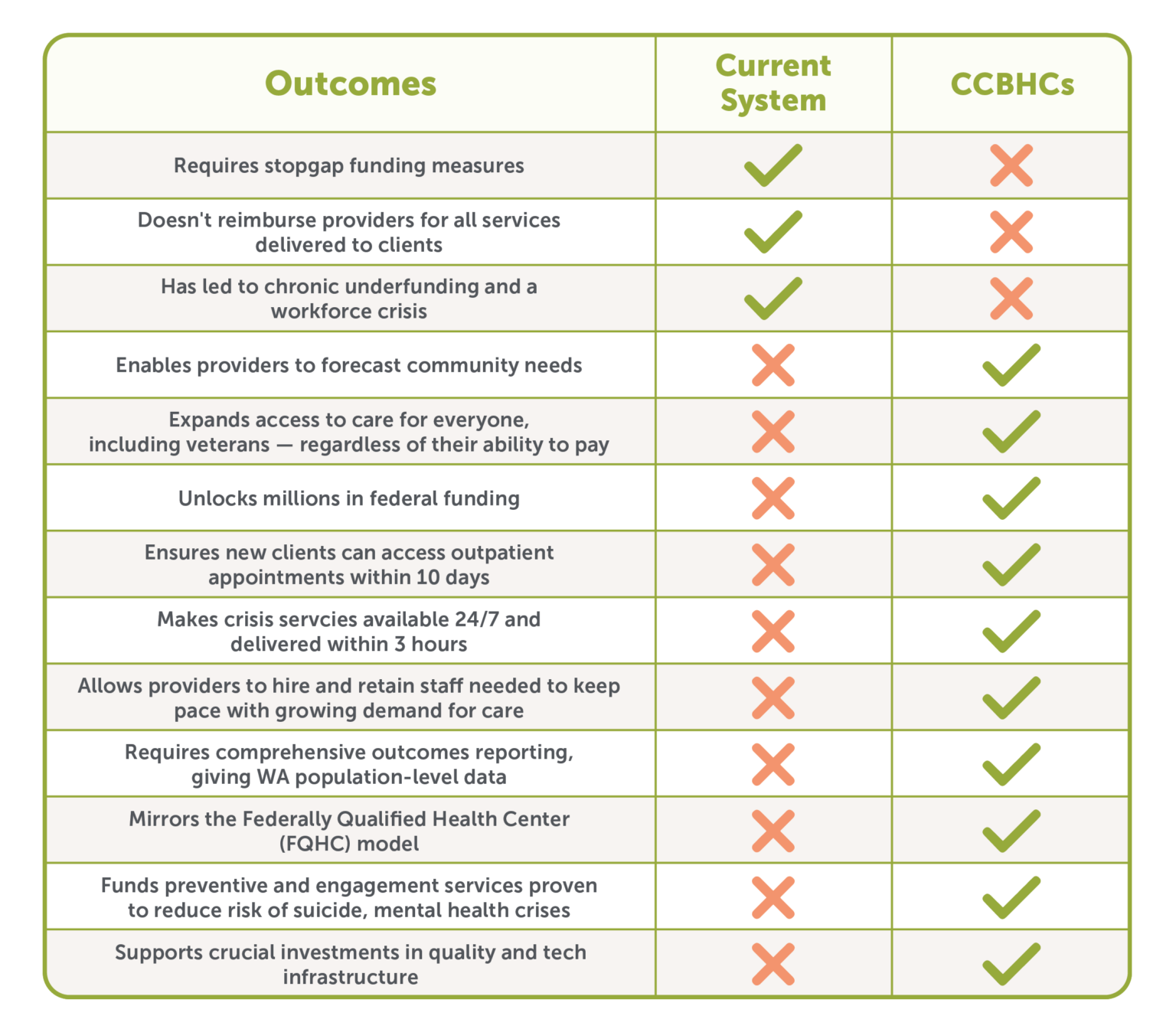
The CCBHC model offers a promising solution for Washington because it will help to:
Demonstrated Success Nationwide
The CCBHC model has yielded game-changing results in early-adopter states.
On average, the 12 states that have implemented the CCBHC model statewide are:
- Serving 25% more behavioral health clients
- Eliminating waitlists and expanding service lines
- Hiring and retaining enough staff to keep pace with demand
The Prospective Payment System Difference
Currently, most providers are compensated on a “fee-for-service” model -which is retrospective, and doesn’t reimburse providers for all the services they deliver. The CCBHC funding mechanism – the Prospective Payment System (PPS) – takes a real-world approach, enabling providers to forecast community needs and secure adequate funding to meet them.
Importantly, PPS funds programs and roles that are simply not accounted for under our current system – because there’s no billing code for them. This means that, through CCBHCs, essential activities that providers are currently delivering for free, including engagement and preventive services, would not only be appropriately funded, but highly encouraged as they promote whole-person health.
For example, in Central Washington, Comprehensive Healthcare has used its CCBHC planning, demonstration and implementation (PDI) grant funding to hire engagement specialists to help ensure clients remain connected to services as they’re leaving inpatient or crisis care. Research shows this is an especially critical time: poor care transitions increase the risk for death by suicide by 200 times in the first month after discharge, and 300 times in the first week. Comprehensive Healthcare’s engagement specialists address barriers that might prevent clients from making an appointment to keep them engaged in services as they continue their journey to recovery.
CCBHC Readiness
As Washington transitions to a CCBHC framework, providers across the state will need to ensure that our people, processes and platforms are prepared to implement federal requirements, many of which require modern infrastructure.
Providers are implementing same-day scheduling and care coordination, opening clinics and major capital projects, and launching other programs to meet CCBHC requirements – well before they are required. CCBHC demonstration grants directly fund these efforts at select agencies, while others are finding alternative paths to readiness.
Fourfront Contributor is also working with state leaders, policymakers and our colleagues to raise awareness and funding for technology modernization and other tools we’ll need to be CCBHC-ready.
We’re advocating for pilot programs that will enable our team members to use AI solutions for administrative tasks, increasing our capacity to focus on client care and supporting staff retention. We’re also testing new software and cloud-based tools that will streamline legacy systems and improve security.
For ongoing updates on how innovative care models and technology will power our efforts to serve communities, visit our news page